What Is Vaginal Cancer?
Vaginal cancer is a malignant tumor arising from vagina. Primary vaginal cancer is rare in the general population of women and is usually a squamous-cell carcinoma. Metastases are more common. Vaginal cancer can be spread from cervical cancer, endometrial cancer, ovarian cancer and choriocarcinoma, besides, cancer cells originating from bladder, urethra, or rectal can often spread to vagina.
Who is at High risk?
Women at age of 60~65 years old.
Young women taking estrogen during pregnancy may cause vaginal clear cell carcinoma.
Women who are with early marriage, early child-bearing and with many times of child-bearing are high-risk groups of primary vaginal cancer.
Women who have multiple sexual partners.
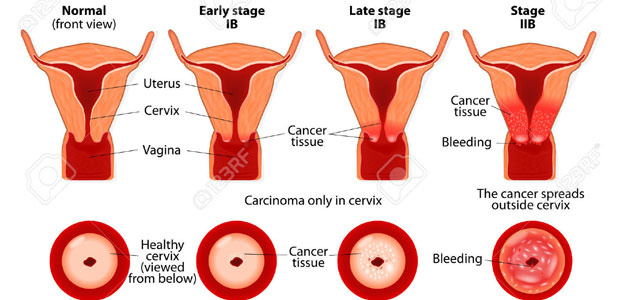
Staging of Vaginal Cancer
Stage 0 vaginal carcinoma in situ
Stage I cancer is confined to the vaginal wall
Stage II cancer has invaded tissues around vagina, but it has not invaded pelvic wall
Stage III cancer has reached pelvic wall
Stage IV cancer has been spread beyond true pelvis or it has invaded bladder, rectum mucosa of rectum, etc
Stage Iva cancer has invaded the adjacent organs
Stage IVb cancer has spread to distant organs
What are the Symptoms of Vaginal Cancer?
How to Diagnose Vaginal Cancer?
What are the Treatments for Vaginal Cancer?
What are the indications of postoperative nursing for patients with vaginal cancer?
When putting into the vagina speculum, action should be light, turning the speculum slowly, so as not to damage the cancer tissue, causing massive bleeding.
Patients with menstrual period or vaginal bleeding are forbidden from douching, in order to prevent intrauterine infection.
Solution concentration for douche should be accurate and temperature should be appropriate, generally 38 ~41 ℃.
Douching pressure should be appropriate. If pressure is excessive, douching solution is easy to flow into uterine cavity, but if pressure is too small, there will no effect for douche.
Observe the changes of patient’s condition. If there is continuous or massive bleeding, douche should be immediately stopped and gauze should be tamped into vagina, informing physicians to cope with it.
For patients with swelling, congestion, ulcer of genital or vaginal stenosis, a miniature speculum should be used to douche so as to relieve patient’s pain.
Douching should be changed every day and the washing barrel should be brushing and disinfected 1 times weekly.