For Endy, a resident of Surabaya, Indonesia, 2021 was the heaviest year of his life.
At 52, he had always been fairly healthy, but began to feel a dull discomfort in his upper abdomen. At first, he thought it was just a minor stomach issue and didn't pay much attention. However, the test results at his local hospital left him and his family in shock — a mass was found in the tail of the pancreas, and it had already invaded the spleen.
Doctors recommended immediate surgery. He underwent a distal pancreatectomy with splenectomy. Postoperative pathology confirmed pancreatic ductal adenocarcinoma — known as the "king of cancers" for its high recurrence rate and rapid progression.
Surgery was only the beginning. He then completed systemic adjuvant chemotherapy and entered a long-term follow-up phase. During that time, his life was filled with constant check-ups and waiting for results.
He thought everything was under control.
But the turning point in the fate often comes without a sound.
Alarming Follow-Up: Abdominal Lymph Node Metastasis
An imaging examination at the end of 2024 shattered the calm.
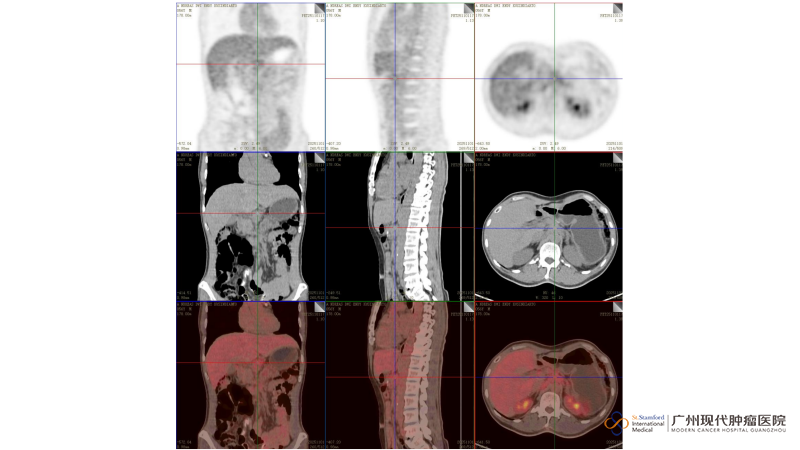
Pre-treatment CT image of Mr. Endy
The images revealed new lymph node shadows in the abdomen with metabolic activity (SUV ~3.0). Doctors warned of a high suspicion of metastasis — the cancer might have returned.
Local doctors offered a dilemma: the lymph nodes were located close to major blood vessels, making conventional treatment difficult to target precisely, with an uneasy balance between risk and benefit.
Endy’s hands trembled as he flipped through the report. One thought kept circling in his mind: I’ve already had my pancreas and spleen removed. Do I need another surgery?
Should he stick with limited conventional options, or seek new possibilities? His family frantically searched for treatments — until they came across four words: **minimally invasive interventional therapy**.
Flying to Guangzhou, Betting on a Possibility
Online, Endy's family learned about the minimally invasive interventional therapy offered at Modern Cancer Hospital Guangzhou. This approach — "without major open surgery" — delivers drugs directly to the tumor's blood supply area for precise treatment, while causing relatively less overall damage to the body. For Endy, who had already undergone major surgery and had limited physical reserve, this was especially important.
However, flying to a foreign country for treatment was not an easy decision. What if there was a language barrier? What if the treatment plan deviated from expectations? What if the results were not as hoped — would the journey be worth it? In the nights before departure, Endy and his family discussed these questions over and over, their hearts filled with both hope and heavy uncertainty.
In November 2025, Endy, accompanied by his family, flew from Surabaya, Indonesia, to Guangzhou. The moment he stepped off the plane, the unfamiliarity of a foreign country struck him — different language, different sounds, different streets — everything instinctively put him on edge.
But as soon as he walked through the doors of Modern Cancer Hospital Guangzhou, that tension began to ease. The hospital assigned dedicated staff to receive him, with interpreters accompanying him throughout. From registration and consultations to various examinations, every step was patiently explained in a language he understood. The doctors did not rush into discussing treatment; instead, they carefully reviewed all the medical records he had brought, and explained the current condition and possible interventional options in a way he could clearly understand.

Endy with his wife
Endy later recalled, "Before coming, my biggest fear was not understanding what was being said or what would happen next. But by the end of the first day, that anxious feeling in my heart had mostly faded away."
Five Treatment Sessions Completed – The Evidence in the Images
After a thorough assessment of Endy's condition, the hospital's multidisciplinary team (MDT) of experts developed a comprehensive plan: first, interventional arterial infusion chemotherapy (HAIC) to shrink the abdominal metastatic lymph nodes, followed by seed implantation to promote tumor necrosis.
In November 2025, Endy received his first session of interventional arterial infusion chemotherapy combined with radioactive seed implantation. From then until February 2026, he persevered through and completed subsequent consolidation therapy. Follow-up imaging after treatment showed that the abdominal metastatic lymph nodes had significantly shrunk, with markedly reduced metabolic activity. The disease has been effectively brought under control, and the patient is generally in good condition.
Treatment is not achieved overnight; it is a prolonged battle.
From November 2025 to February 2026, Endy completed several sessions of systemic therapy and received precise localized radioactive seed implantation. After each treatment, he would walk a few laps in the hospital corridor and greet the nurses with simple Chinese phrases. Gradually, Modern Cancer Hospital Guangzhou was no longer just an "unfamiliar treatment place" to him, but a place where he felt "someone truly cares about me."
The PET-CT follow-up on January 30, 2026, brought encouraging results. Compared with the CT images from November 2025: the multiple lymph node shadows and patchy density increases in the retroperitoneal and hepatic portal regions had significantly reduced in size and showed markedly decreased metabolic activity. The largest lesion, previously measuring approximately 3.6 cm × 3.3 cm × 3.5 cm (SUVmax 3.3), had shrunk to 1.0 cm × 0.9 cm after treatment, with significantly reduced metabolic activity and no abnormal findings in some areas.
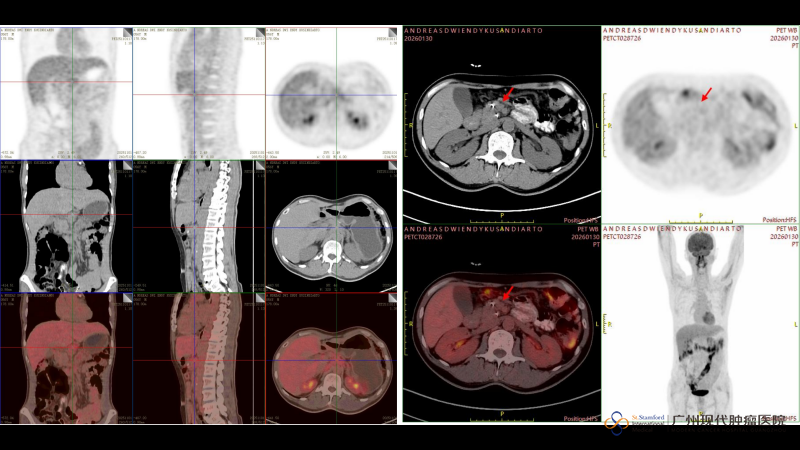
Left: November 1, 2025 – Before treatment, the lesion measured approximately 3.6cm × 3.3cm × 3.5cm at its largest.
Right: January 30, 2026 – After treatment, the lesion shrank to 1.0cm × 0.9cm.
Doctor's assessment:
Tumor activity has been significantly suppressed, and the overall disease is effectively controlled.
What reassured the family even more was that Endy had no significant weight loss, his diet and sleep were acceptable, and his general condition remained good. Pancreatic cancer patients often lose weight rapidly due to malabsorption and tumor consumption. Therefore, stable weight itself is an important sign of disease control.

Mr. Endy and his family with the hospital's specialists and nurses
Expert Commentary: How Interventional Therapy Helps Defeat Pancreatic Cancer

Dr. Lin Jing, Deputy Director of the International Oncology Ward at Modern Cancer Hospital Guangzhou
Dr. Lin Jing, Associate Chief Physician, emphasized that pancreatic cancer is a long-term battle. With consistent standardized treatment, regular follow-up, and good nutritional support, even if metastasis occurs, there remains a chance to keep the disease under long-term control and maintain a good quality of life.
When the disease is stabilized, life can go on
Endy admitted that when he first received the metastasis report, his hands trembled so much he could barely hold the paper. "Were all my previous sufferings for nothing?" That thought weighed on his heart like a stone.
But as treatment progressed, the lesion shrank from 3.6 cm to 1 cm, and his body held up — he could eat, sleep, and take walks in the corridor. These small yet real signs of "normal life" gradually pulled him back from the depths of despair.
Now the patient, Endy, is in good spirits, eating and sleeping normally, while continuing oral maintenance medications and regular follow-ups. From trembling hands and silence when he first received the metastasis report, to now being able to calmly share his treatment journey, his transformation is not just physical but also mental. He said, “I used to think pancreatic cancer meant waiting for death. Now I believe that with the right approach, you can truly survive.”
These words are the best response to all the struggles, anxieties, and perseverance of the past few months.
The disease may not be easily reversed, but it can be controlled — and life can still move forward. Endy’s story proves one thing: where the disease stands does not mean where life stops. The key is finding the right path.
No matter how tough the cancer, it fears a person who refuses to give up. No matter how advanced the disease, it fears the right treatment plan. Don’t lose hope. Even in late stages, a turning point is possible.
*Surgery, in addition to the appropriate chemotherapy and radiotherapy, are effective in treating early cancer, but certain patients in late stage of cancer may not be tolerate surgery well as they can be relatively weak. A combination of carefully planned minimally invasive therapy, chemotherapy or radiotherapy can effectively reduce the side effects and discomfort of treatment and may help patient get better efficacy.













 viber
viber